Development of IgG food allergies
From a damaged gut to chronic inflammation
When you are suffering from a condition that will just not go away, the cause may be a delayed IgG food allergy (type III). IgG food allergies often remain undetected because the symptoms only occur a few hours or even days after the consumption of a trigger food. This makes them extremely difficult to identify. Fortunately, a reliable diagnostic test and nutritional concept can help: ImuPro.
The immune system of the intestine
The immune system of the intestine is the largest in the entire body. Over 80% of the immune defence reactions have their origin in the intestine. It guarantees an almost invincible barrier for bacteria, viruses and other disease pathogens and a barrier against other foreign proteins from food. Foods have an extraordinary tolerance, on condition that they are correctly digested and pass the intact intestinal mucous membrane in the planned manner, namely through the intestinal cells.
An intact gut barrier is the key for tolerance. Learn how a damaged gut barrier may result in chronic inflammation in the following four steps.
What are the possible symptoms
- Gastrointestinal ailments like bloating, constipation, diarrhoea, nausea, Crohn’s Disease, Irritable Bowel Syndrome (IBS)
- Headaches, migraines
- Obesity, chronic weight problems
- Atopic dermatitis-like skin problems, psoriasis, eczema
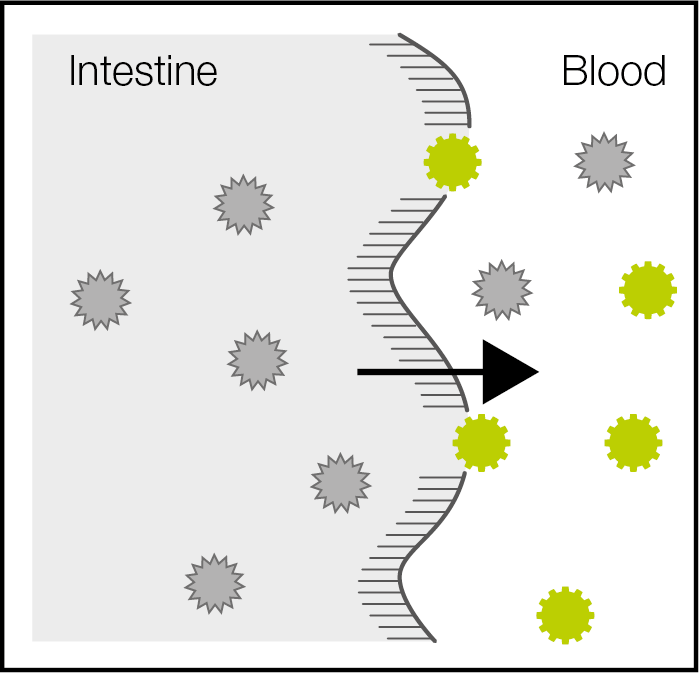
Damage to the intestine results in incorrect identification
Due to medicines, infections, mycosis, stress and environmental poisons, the integrity of the intestinal wall can be damaged and food components can slip between the intestinal cells.
Food that passes through the intestinal cells is correctly digested and tolerated by the immune system. In contrast, food that passes by the intestinal cells might be recognised as foreign. An immune reaction is then initiated in order to destroy the invading proteins (see Step 2).
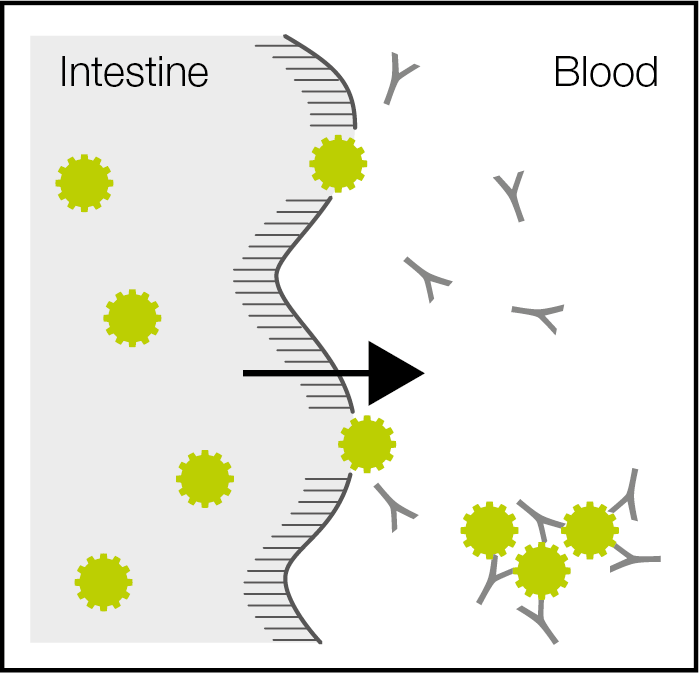
Immune response causes inflammatory conditions
In contrast to infectious agents like bacteria, viruses, moulds and parasites and because food normally doesn’t present a threat to the organism, food is not recognized by the innate immune system, but by the adaptive immune system.
It produces IgG antibodies which recognise the food for which they have been formed. These antibodies are also transferred from mother to baby in the 3rd trimester of pregnancy.
The IgG antibodies fix to the food proteins to form an immune complex. In the blood stream they are called circulating immune complexes. The complement system then initiates the destruction of the immune complexes through immune cells (neutrophils). When the immune cells destroy the complexes, an inflammatory reaction takes place.
The inflammatory reaction may result in unspecific symptoms (e. g. fatigue) or in specific symptoms (e. g. migraine). This depends on where the immune complex is destroyed (see Step 3 and Step 4).
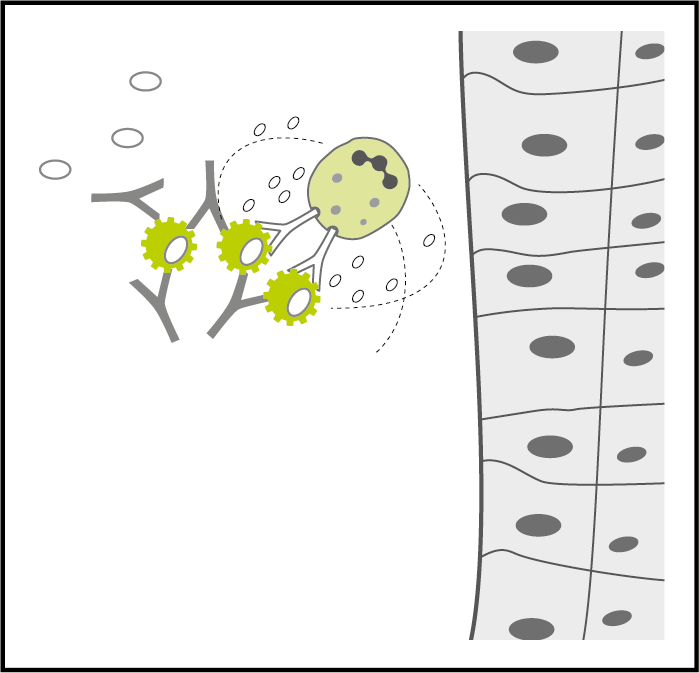
Destruction in circulation may result in unspecific symptoms
If the immune complexes are destroyed in circulation, you may not experience any specific symptoms. Unspecific symptoms can be fatigue and retention of water, reflected by an unexplained variation of body weight. On the long term, systemic symptoms like hypertension or metabolic disorders might develop.
Learn in Step 4 how the destruction of immune complexes may result in specific symptoms.
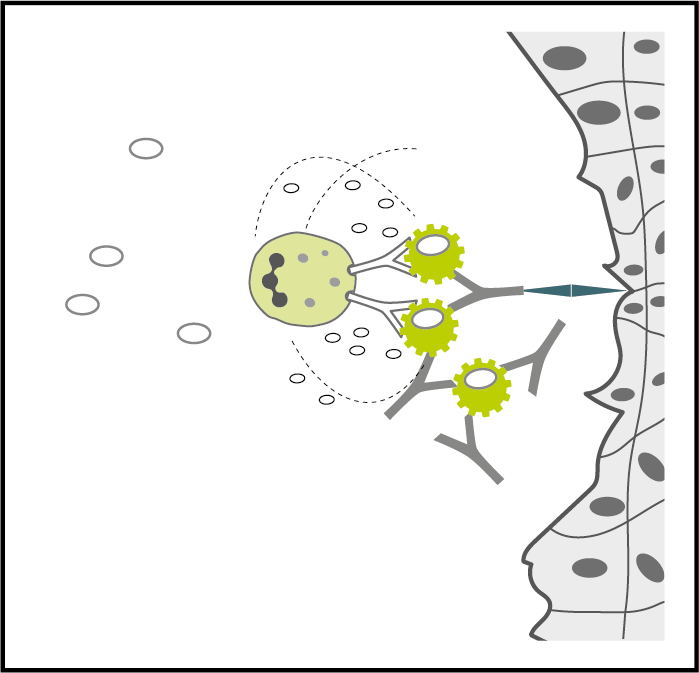
Local destruction may result in specific symptoms
If the immune complex is fixed to a tissue, it is also destroyed, but locally and the surrounding tissue is damaged as well. This may result in specific symptoms like migraine or IBS.
Note: If the food forming the immune complex is eaten regularly, the inflammatory reaction may become chronic. Symptoms (systemic or specific) do not appear immediately. It may take several months before a symptom becomes apparent. Often it starts to appear gradually, but intensifies with time.